Last update 19 Sep 2024
TIGIT checkpoint inhibitor (GigaGen)
Last update 19 Sep 2024
Overview
Basic Info
Originator Organization |
Active Organization- |
Inactive Organization |
Drug Highest PhasePendingDiscovery |
First Approval Date- |
Regulation- |
Related
100 Clinical Results associated with TIGIT checkpoint inhibitor (GigaGen)
Login to view more data
100 Translational Medicine associated with TIGIT checkpoint inhibitor (GigaGen)
Login to view more data
100 Patents (Medical) associated with TIGIT checkpoint inhibitor (GigaGen)
Login to view more data
13
Literatures (Medical) associated with TIGIT checkpoint inhibitor (GigaGen)01 May 2024·Science China Life Sciences
Hemin blocks TIGIT/PVR interaction and induces ferroptosis to elicit synergistic effects of cancer immunotherapy
Article
Author: Zhang, Xiangrui ; Li, Beibei ; Wu, Menghan ; Zhai, Wenjie ; Wu, Yahong ; Li, Yang ; Li, Guodong ; Zhou, Xiuman ; Jin, Shengzhe ; Dong, Qingyu ; Du, Jiangfeng ; Zhou, Xiaowen ; Qiu, Lu ; Qi, Yuanming ; Gao, Yanfeng ; Zhao, Wenshan
21 Mar 2024·NatureQ1 · CROSS-FIELD
Anti-TIGIT antibody improves PD-L1 blockade through myeloid and Treg cells
Q1 · CROSS-FIELD
Article
Author: Felip, Enriqueta ; Duong, Ellen ; Hendricks, Robert ; Molden, Nandini ; Mellman, Ira ; Han, Chia-Jung ; Mittman, Stephanie ; Silva, John ; Abreu, Delvys Rodriguez ; Johnston, Robert J ; Guan, Xiangnan ; Nabet, Barzin Y ; Daggumati, Pallavi ; Mariathasan, Sanjeev ; Choi, Yoonha ; Cho, Byoung Chul ; Meng, Raymond ; McGinnis, Lisa ; Srivats, Shyam ; Dunkle, Alexis ; Nutsch, Katherine ; Gil-Bazo, Ignacio ; Chiang, Eugene Y ; Banta, Karl L ; Chang, Patrick S ; Hu, Ruozhen ; Shames, David S ; Italiano, Antoine ; Connolly, Wendy ; Johnson, Melissa ; Patil, Namrata S
01 Jan 2024·Advanced Biology
TIGIT may Serve as a Potential Target for the Immunotherapy of Renal Cell Carcinoma
Article
Author: Yu, Chengfan ; Hong, Xin ; Bi, Jianlong ; Liu, Qing ; Wang, Qiang
40
News (Medical) associated with TIGIT checkpoint inhibitor (GigaGen)28 Aug 2024
Less than a week after announcing it will merge its cancer immunology and molecular oncology teams under a single umbrella, Genentech filed to begin a round of layoffs at its South San Francisco site. According to a California Worker Adjustment and Retraining Notification (WARN) notice submitted on August 22, the Roche unit will cut 93 positions starting in October. On August 16, Genentech had disclosed plans to restructure its cancer R&D business, dissolving its cancer immunology group as a free-standing entity and prompting the planned departure of Ira Mellman, the company's long-time vice president of cancer immunology.While the company was a pioneer of targeted monoclonal antibodies, it has struggled to keep pace in the rapidly changing immuno-oncology space. Roche's recent setbacks with TIGIT inhibitor tiragolumab have also highlighted the challenges in developing next-generation checkpoint inhibitors (See – Spotlight On: Roche's latest TIGIT implosion - three key takeaways).For a deeper take on the oncology overhaul at Genentech, see – Spotlight On: Roche concedes that immuno-oncology needs a re-think.
ImmunotherapyAcquisition
20 Aug 2024
Merck & Co. is again refining the scope of its antibody-drug conjugate (ADC) pact with Sichuan Kelun-Biotech Pharmaceutical, opting to license the bispecific ADC candidate SKB571, while handing back rights to another asset focused on the CLDN18.2 target.The companies struck a partnership in 2022 in which Merck was granted overseas development rights to the TROP2-targeting ADC asset MK-2870 (SKB-264) for potentially over $1.4 billion. Merck later shelled out another $175 million as part of a heavily backloaded expanded collaboration that could eventually net Kelun over $9 billion.Despite doubling down on ADCs via a massive deal worth up to $22 billion with Daiichi Sankyo late last year, Merck pulled out of developing two preclinical therapies under development with Kelun. The company has now fine-tuned the alliance with the Chinese biotech again.In a release detailing its half-year results, Kelun said Merck has now taken up its option on SKB571 for $37.5 million. Kelun described the programme as primarily intended for solid tumours like lung and gastrointestinal cancers. "Through a scientific selection of target combinations and a differentiated design of [bispecific antibody] molecules, it is designed to enhance tumour targeting and help overcome tumour heterogeneity, thereby improving efficacy," the company said.Preclinical studies of SKB571 have demonstrated "promising anti-tumour efficacy and a good safety profile" in multiple patient-derived xenograft models and cynomolgus monkeys, according to Kelun. The biotech plans to submit an investigational new drug (IND) application for the bispecific ADC "in the near future."Meanwhile, Merck has returned global rights to Kelun's CLDN18.2-directed ADC candidate SKB315. Kelun noted that early-stage clinical data for SKB315 has shown "positive efficacy and acceptable safety profile in GC [gastric cancer] with high CLDN18.2 expression," and the company expects to present findings at upcoming conferences."Given the significant population of GC patients in China, we have confidence in the market prospects of SKB315 in China. We will continue to expedite its development in China and explore suitable expansion into overseas markets," it added.The updates to the Kelun-Merck collaboration come as the broader immuno-oncology (I-O) landscape shows signs of slowing, with Roche recently merging its I-O unit into a broader oncology group amid a series of setbacks for TIGIT inhibitors. See – Vital Signs: Tracking the shrinking returns in I-O, and who has the most to lose.
ADCINDLicense out/in
16 Aug 2024
Genentech, a subsidiary of Roche, confirmed that it is retooling its oncology research activities and will merge its cancer immunology and molecular oncology teams under a single umbrella. The move comes as Ira Mellman, the company's long-time vice president of cancer immunology, prepares to leave after more than 17 years with the biotech pioneer.The restructuring reflects broader shifts in the immuno-oncology landscape, where initial enthusiasm for novel targets like TIGIT has been tempered by disappointing clinical results. See – Spotlight On: Roche's latest TIGIT implosion - three key takeaways.In a statement to FirstWord, Genentech explained that "based on shifts in the science of immuno-oncology, Genentech Research and Early Development (gRED) will unify its cancer immunology and molecular oncology research under a single oncology organisation." In addition, the discovery teams in HPORT (human pathobiology & OMNI reverse translation) will move to the immunology and neuroscience departments within Research Biology.Mellman, who joined Genentech in 2007 and established the cancer immunology group 12 years ago, has been a driving force behind the company's efforts in the field. During his tenure, the team brought Tecentriq (atezolizumab) into clinical development and spearheaded Genentech's entry into cell therapy and personalised cancer vaccines."Ira's impact extends beyond Genentech, as he is widely recognised as an international leader in the field of cancer immunology, having made seminal contributions to our understanding of the immune system and its role in cancer," the company said.The changes raise questions about Genentech's future priorities in oncology research. While the company was an early pioneer of targeted monoclonal antibodies, it has struggled to keep up in the rapidly changing immuno-oncology space. Roche's recent setbacks with TIGIT inhibitor tiragolumab have also highlighted the challenges in developing next-generation checkpoint inhibitors.For a deeper take on the oncology overhaul at Genentech, see – Spotlight On: Roche concedes that immuno-oncology needs a re-think.
Executive ChangeImmunotherapy
100 Deals associated with TIGIT checkpoint inhibitor (GigaGen)
Login to view more data
R&D Status
10 top R&D records. to view more data
Login
| Indication | Highest Phase | Country/Location | Organization | Date |
|---|---|---|---|---|
| Neoplasms | Discovery | US | 19 Dec 2017 |
Login to view more data
Clinical Result
Clinical Result
Indication
Phase
Evaluation
View All Results
| Study | Phase | Population | Analyzed Enrollment | Group | Results | Evaluation | Publication Date |
|---|
No Data | |||||||
Login to view more data
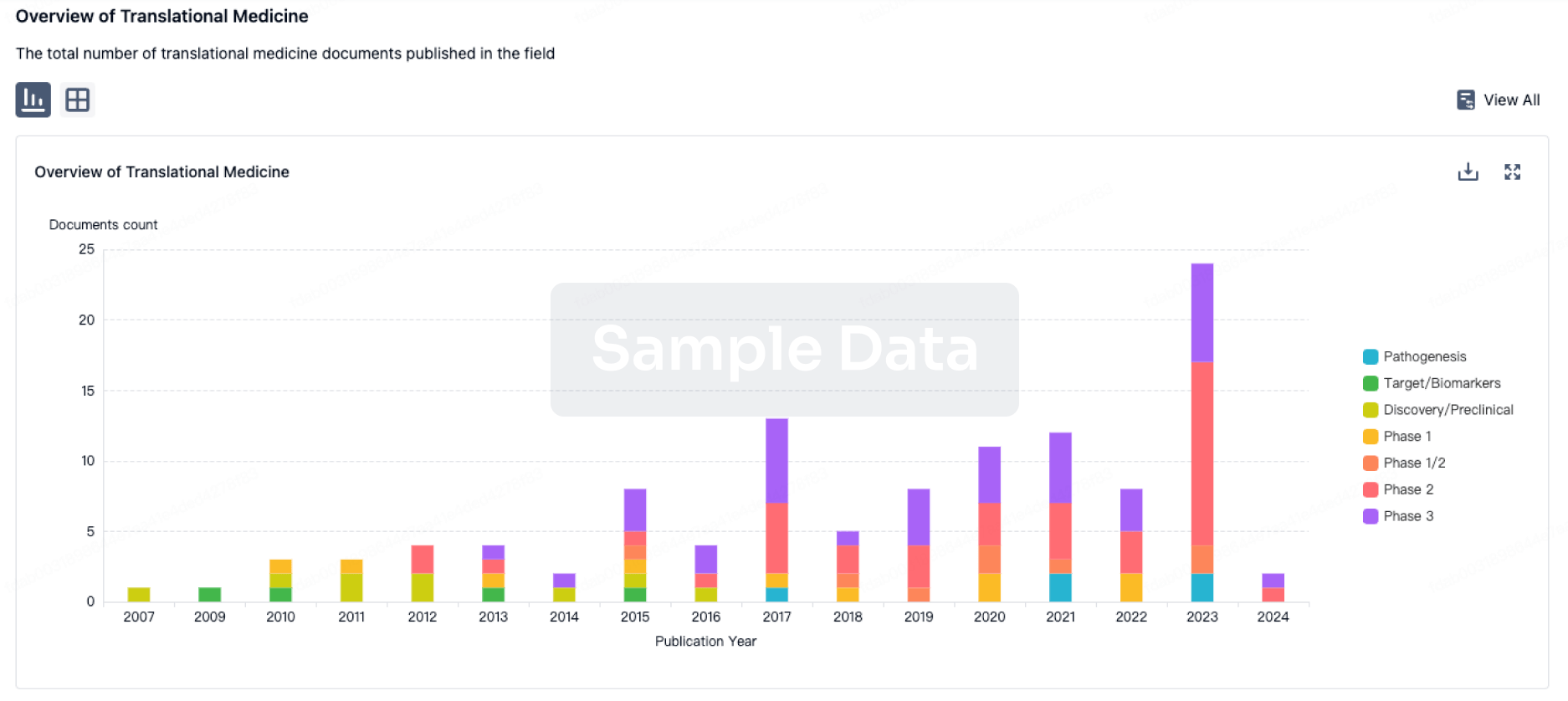
Translational Medicine
Boost your research with our translational medicine data.
login
or
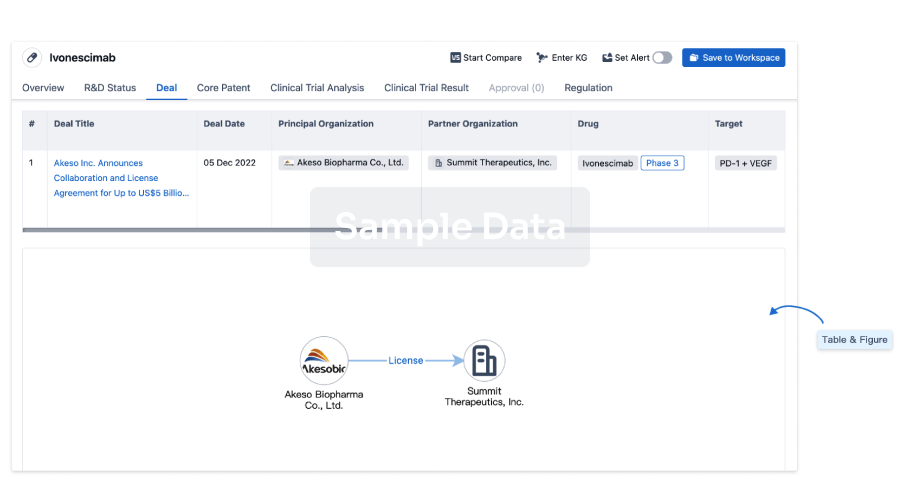
Deal
Boost your decision using our deal data.
login
or
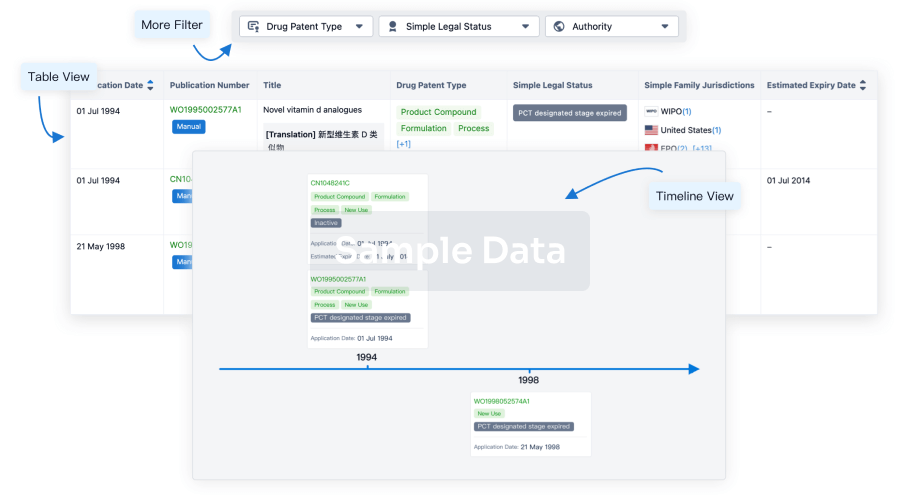
Core Patent
Boost your research with our Core Patent data.
login
or
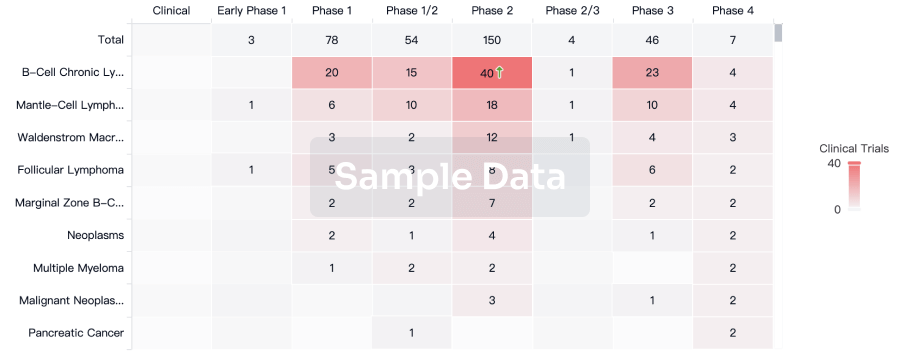
Clinical Trial
Identify the latest clinical trials across global registries.
login
or
Approval
Accelerate your research with the latest regulatory approval information.
login
or
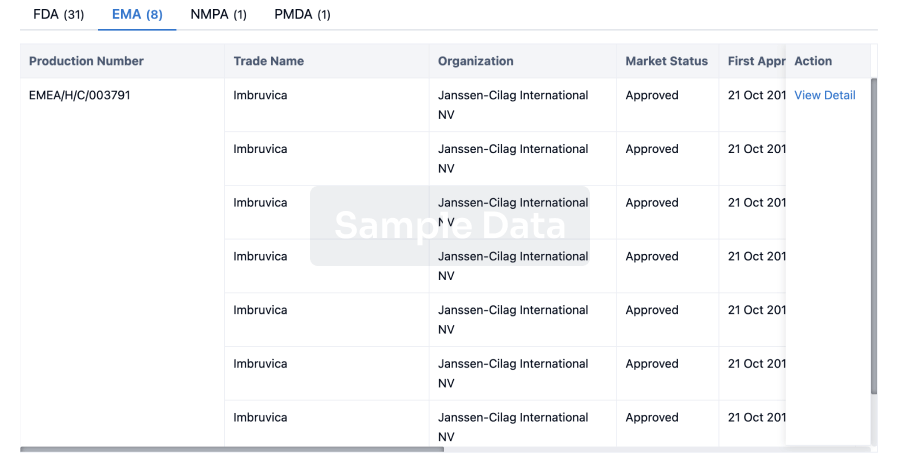
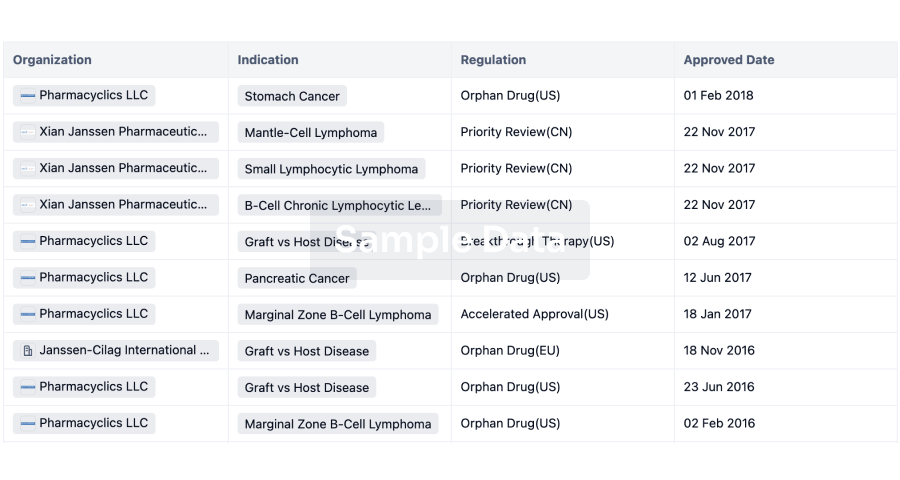
Regulation
Understand key drug designations in just a few clicks with Synapse.
login
or
Chat with Hiro
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free
