Request Demo
Last update 20 Mar 2025
Cytomegalovirus glycoprotein vaccine(GlaxoSmithKline Plc)
Last update 20 Mar 2025
Overview
Basic Info
Drug Type Combination vaccine, Prophylactic vaccine |
Synonyms Cytomegalovirus glycoprotein vaccine, GSK Biologicals' recombinant CMV gB vaccine + [1] |
Target |
Action antagonists |
Mechanism CMV gB antagonists(CMV gB antagonists) |
Therapeutic Areas |
Active Indication |
Inactive Indication- |
Login to view timeline
R&D Status
10 top R&D records. to view more data
Login
| Indication | Highest Phase | Country/Location | Organization | Date |
|---|---|---|---|---|
| Cytomegalovirus Infections | Phase 2 | United States | 14 Oct 2021 |
Login to view more data
Clinical Result
Clinical Result
Indication
Phase
Evaluation
View All Results
Not Applicable | 47 | Blood sampling+GSK149203A (GSK149203A S- Group) | bhssozppmi(vkzzgnxrxk) = kabznxjrln tlwkvoaxhg (gsfxosmgmw, pelubtoebn - vbnocmgdtx) View more | - | 06 Oct 2017 | ||
Blood sampling (GSK149203A S+ Group) | rroinewcdw(leyjmkmhsg) = aezpopibnf mopdbgqemn (vnxqoohaoy, udrlofycgh - kfdnpbimzk) View more |
Login to view more data
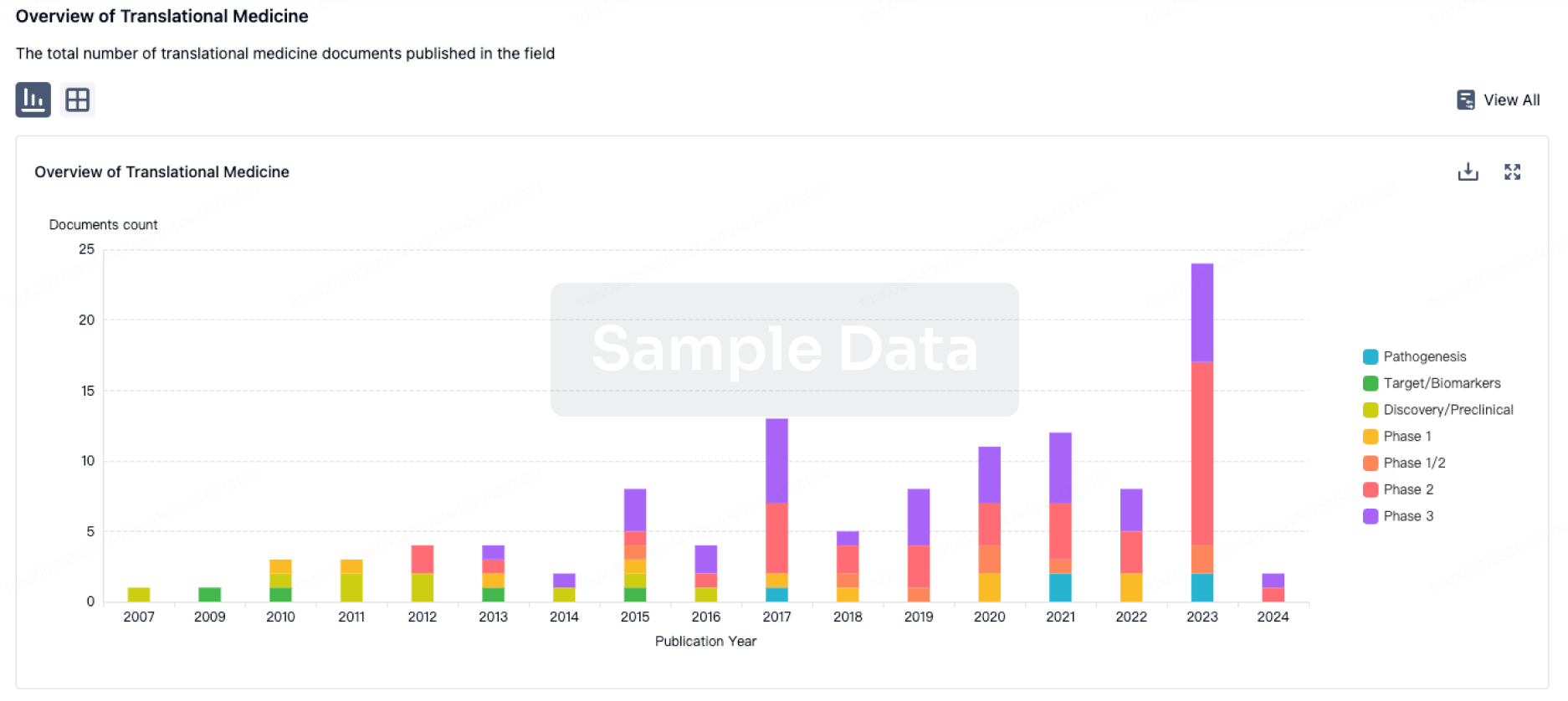
Translational Medicine
Boost your research with our translational medicine data.
login
or
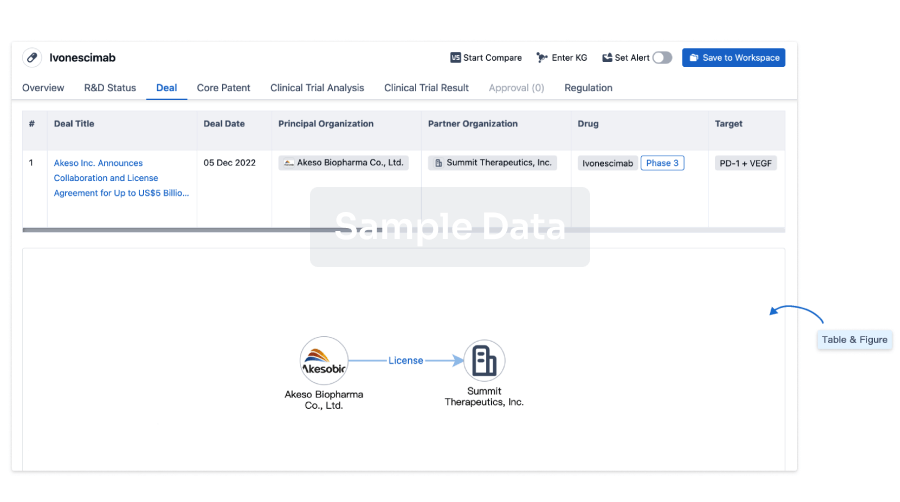
Deal
Boost your decision using our deal data.
login
or
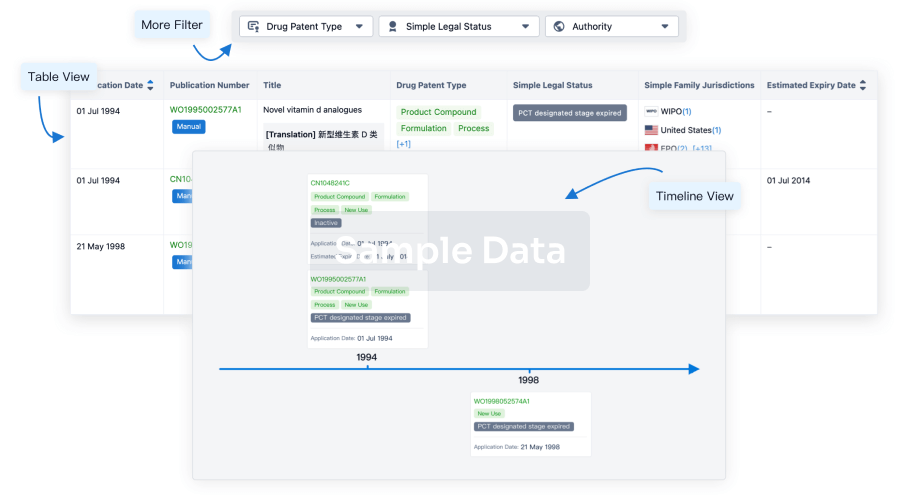
Core Patent
Boost your research with our Core Patent data.
login
or
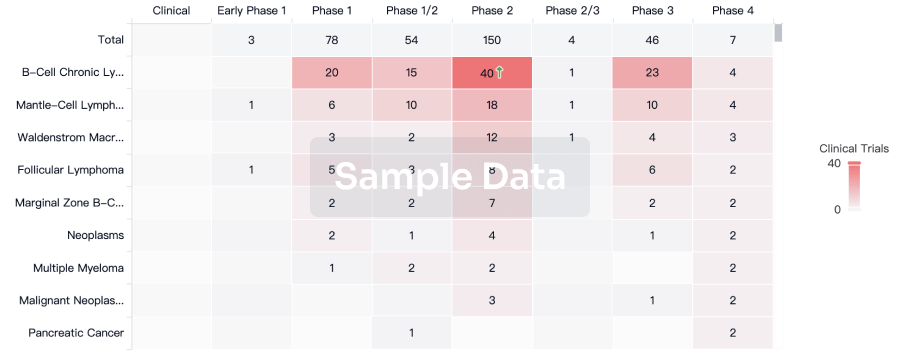
Clinical Trial
Identify the latest clinical trials across global registries.
login
or
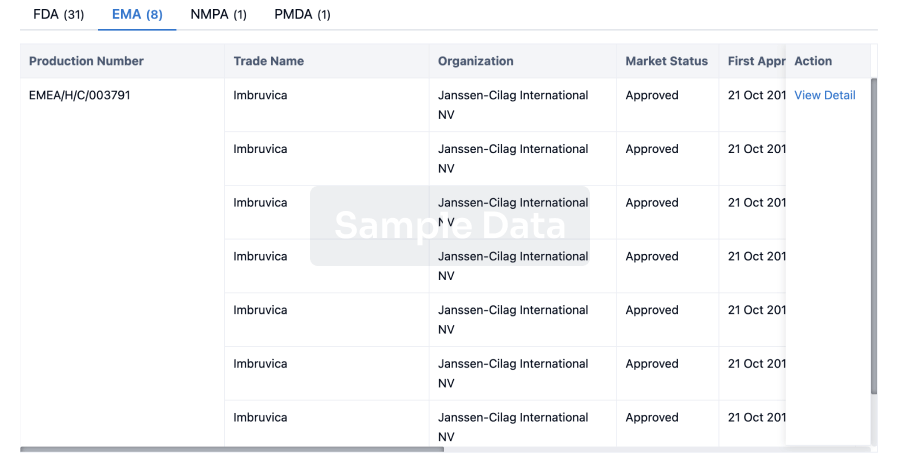
Approval
Accelerate your research with the latest regulatory approval information.
login
or
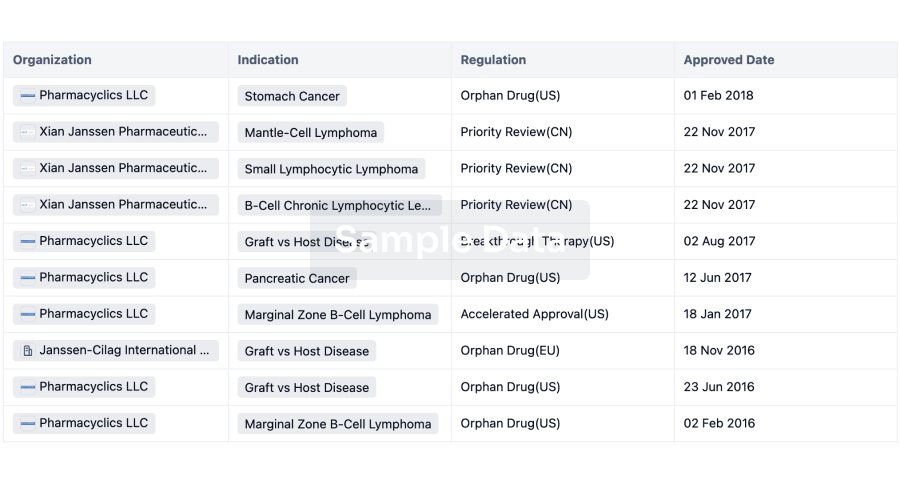
Regulation
Understand key drug designations in just a few clicks with Synapse.
login
or
Chat with Hiro
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free
