Last update 28 Sep 2024

Orthopedic ONE
Last update 28 Sep 2024
Overview
Related
2
Clinical Trials associated with Orthopedic ONERandomized Controlled Trial of Home-based Physical Therapy Versus Outpatient Clinic-based Physical Therapy Following Primary Anterior Total Hip Arthroplasty
130 patients undergoing primary unilateral total hip arthroplasty through anterior approach were enrolled and randomized into one of two groups. One group received standard of care clinic-based physical therapy postoperatively (clinic PT) while the other group underwent progressive home-based exercises to do after surgery (home PT). Patient surveys with Hip Osteoarthritis Outcome Scores (HOOS) and SF12v2 scores for both groups were obtained before surgery as well as 6, 14, and 24 weeks postop. Patients had the option to crossover into the other study group at their 6-week follow-up visit.
Start Date31 Jul 2018 |
Sponsor / Collaborator  Orthopedic ONE Orthopedic ONE [+1] |
The Use of Teriparatide as an Adjunctive Therapy for the Treatment of Jones Fractures
This randomized, placebo-controlled study will evaluate the effectiveness of the adjunctive use of teriparatide for the healing of Jones fractures.
Start Date01 Jul 2010 |
Sponsor / Collaborator |
100 Clinical Results associated with Orthopedic ONE
Login to view more data
0 Patents (Medical) associated with Orthopedic ONE
Login to view more data
8
Literatures (Medical) associated with Orthopedic ONE01 Oct 2014·The Journal of bone and joint surgery. American volumeQ2 · MEDICINE
Associations Between Preoperative Physical Therapy and Post-Acute Care Utilization Patterns and Cost in Total Joint Replacement
Q2 · MEDICINE
Article
Author: Vogel, Karen ; Granata, Jaymes ; Ruhil, Anirudh V S ; Wasielewski, Ray ; Snow, Richard ; McShane, Michael
BACKGROUND:
Health-care costs following acute hospital care have been identified as a major contributor to regional variation in Medicare spending. This study investigated the associations of preoperative physical therapy and post-acute care resource use and its effect on the total cost of care during primary hip or knee arthroplasty.
METHODS:
Historical claims data were analyzed using the Centers for Medicare & Medicaid Services Limited Data Set files for Diagnosis Related Group 470. Analysis included descriptive statistics of patient demographic characteristics, comorbidities, procedures, and post-acute care utilization patterns, which included skilled nursing facility, home health agency, or inpatient rehabilitation facility, during the ninety-day period after a surgical hospitalization. To evaluate the associations, we used bivariate and multivariate techniques focused on post-acute care use and total episode-of-care costs.
RESULTS:
The Limited Data Set provided 4733 index hip or knee replacement cases for analysis within the thirty-nine-county Medicare hospital referral cluster. Post-acute care utilization was a significant variable in the total cost of care for the ninety-day episode. Overall, 77.0% of patients used post-acute care services after surgery. Post-acute care utilization decreased if preoperative physical therapy was used, with only 54.2% of the preoperative physical therapy cohort using post-acute care services. However, 79.7% of the non-preoperative physical therapy cohort used post-acute care services. After adjusting for demographic characteristics and comorbidities, the use of preoperative physical therapy was associated with a significant 29% reduction in post-acute care use, including an $871 reduction of episode payment driven largely by a reduction in payments for skilled nursing facility ($1093), home health agency ($527), and inpatient rehabilitation ($172).
CONCLUSIONS:
The use of preoperative physical therapy was associated with a 29% decrease in the use of any post-acute care services. This association was sustained after adjusting for comorbidities, demographic characteristics, and procedural variables.
CLINICAL RELEVANCE:
Health-care providers can use this methodology to achieve an integrative, cost-effective, patient care pathway using preoperative physical therapy.
01 Sep 2013·Orthopedic nursingQ4 · MEDICINE
Q4 · MEDICINE
Article
Author: Latshaw, James C ; Price, Matthew C ; Horn, Pamela L
Proximal humerus fractures are among the most common fractures associated with osteoporosis. With an aging population, incidence of these fractures will only increase. The proximal humerus not only forms the lateral portion of the shoulder articulation but also has significant associations with musculoskeletal and neurovascular structures. As a result, fractures of the proximal humerus can significantly impact not only the function of the shoulder joint, but the health and function of the entire upper extremity as well. Understanding of these fractures, the management options, and associated nursing care, can help reduce morbidity rate and improve functional outcomes.
25 Jul 2012·JBJS case connector
A Sixty-One-Year-Old Woman with Ischemia After Total Knee Arthroplasty
Article
Author: Wilmoth, Jill C ; McShane, Michael A ; Ng, Vincent Y
Arterial complications after total knee arthroplasty are rare, but potentially devastating. Most cases are attributable to predisposing patient risk factors and iatrogenic trauma or manipulation1. Numerous causes, such as thrombosis, vessel severance, aneurysm, and plaque embolization, have been reported in the literature1-4, and the anatomic relationships in the popliteal fossa have been well-described5. We present a case of acute ischemia after total knee arthroplasty associated with position-dependent occlusion of the popliteal artery. The contributing factors included a common underlying patient condition and a frequently used femoral component design. Orthopaedic surgeons that perform total knee arthroplasty regularly should be cognizant of the hallmark presentation of this complication, the appropriate clinical workup, and the optimal treatment options. The patient was informed that data concerning the case would be submitted for publication, and she provided consent.
A sixty-one-year-old woman presented with acute right leg ischemia in the postoperative recovery unit after routine cemented total knee arthroplasty for osteoarthritis. She had symptoms of marked pain and weakness throughout the leg. Surgery had been performed via a standard medial parapatellar approach with a tourniquet in place. An LPS-Flex Fixed Bearing implant system (Zimmer, Warsaw, Indiana) with a size 5 tibial baseplate, 29-mm patella, 14-mm polyethylene insert, and size F gender-specific femoral component had been used. Preoperative templating for size and alignment as well as intraoperative bone resection had been facilitated by the Patient Specific Instrumentation (PSI) system (Zimmer). The posterior osteophytes had been removed to achieve full knee extension, and soft-tissue balancing had included subperiosteal elevation of the posterior oblique ligament, deep medial collateral ligament, and semimembranosus tendon insertion.
The patient’s medical history included hypertension, coronary artery disease, and carotid artery disease. She denied exertional chest pain or lower-extremity claudication. The remainder of the history was noncontributory. …
6
News (Medical) associated with Orthopedic ONE10 Oct 2023
VUZE 2.0 designed to provide extended functionality, broader inter-operability while still requiring no tool modifications, cameras, markers or references
RA’ANANA, Israel--(BUSINESS WIRE)-- VUZE Medical, a privately-held company aiming to transform intra-operative guidance in minimally invasive spinal interventions, has submitted a 510(k) filing with the U.S. Food and Drug Administration (FDA) for VUZE 2.0, its second generation VUZE System. The new, investigational version of the VUZE System will be featured prominently at NASS 2023, the 38th annual meeting of the North American Spinal Society, which will be held October 18-21 in Los Angeles.
The VUZE System is a software solution installed on an off-the-shelf PC. It operates with unmodified surgical tools, requires no markers, references or cameras, and with no need for 3D imaging within the operating room (OR). Using proprietary image processing, it overlays in real time graphical representations of standard surgical tools seen in intra-operative 2D X-ray images onto axial and sagittal cross-sections that it generates from the patient’s standard pre-operative 3D scan. The VUZE System previously received U.S. FDA 510(k) clearance in 2022 and completed a successful first-in-human clinical trial in early 2023. VUZE Medical has received eight related patents to date in the U.S., Europe and Asia.
Attendees of NASS 2023 will have the opportunity to observe the investigational VUZE 2.0 in cadaveric surgery in a Surgical Stadium session titled “Navigated MISS with No Tool Modifications, References, Markers or Cameras” on October 19 from 11 a.m. to 12 p.m. PT. Hands-on experimentation will be available at a cadaveric workshop on October 19 from 1 to 4 p.m. PT. Further information will be provided at the VUZE Medical booth #1051. Clinical experience will be reviewed in a Red Theater Presentation, “A New Approach to Guidance and Verification in MISS: Results of First-in-Human Trial with the VUZE System,” on October 20 from 1 to 1:20 p.m. PT.
The second generation VUZE System is designed to support a broader range of surgical C-arms from multiple vendors and accommodate more sources of 3D image data, including both pre-operative CT and in-OR 3D scans. It also aims to provide expanded functionality, including the ability to perform surgical planning on a standalone laptop in addition to on the VUZE System.
“Our second generation aims to extend the operability of the VUZE System across a much larger percentage of operating rooms,” said David Tolkowsky, founder and CEO of VUZE Medical. “The new features and functionality could, once cleared by FDA, make VUZE more accessible and provide surgeons with more effective guidance in situations where they previously did not have many attractive options.”
Over three million surgeries for correcting spinal instability and/or deformation, collectively known as spinal stabilizations, are performed annually worldwide, with a third of those in the U.S.1 These procedures include vertebral fixation with pedicle screws, vertebral fixation coupled with fusion, and vertebral augmentation with synthetic or biological cement. Approximately 80 percent of stabilizations treat short spinal segments 1. Short-segment surgeries are most often performed manually and are typically assisted only by standard 2D X-ray.
About VUZE Medical
VUZE Medical is a privately-held medical technology company that aims to provide highly accurate and cost-effective surgical guidance for common spinal interventions currently aided only by standard 2D X-Ray. The company’s VUZE System is a unique software-based solution that instantly merges intra-operative X-ray with pre-operative CT, providing surgeons with the cross-sectional images they need most during surgery and currently lack. The system is targeted primarily at outpatient and ambulatory settings. For more information, visit .
1. Orthopedic Network News: 2020 Spinal Surgery Update
Clinical Study
13 Apr 2023
FDA inspections part of approval process for TOPS facet joint replacement system for lumbar arthroplasty
NORWALK, Conn.--(BUSINESS WIRE)-- Premia Spine, a medical technology company changing the way debilitating chronic leg and back pain is treated, today announced the U.S. Food and Drug Administration (FDA) has completed four Bioresearch Monitoring (BIMO) inspections as part of the PMA approval process for the TOPS facet joint replacement system. The inspections at two company facilities and two clinical trial sites in the U.S. resulted in no FDA Form 483s for objectionable observations.
“While a completely clean site inspection is what everyone strives for, it is a major accomplishment to receive no 483s across four separate sites,” said Ron Sacher, CEO, Premia Spine. “The successful outcomes and completion of the site visits move us one step closer to approval of the TOPS facet joint replacement system, and our goal of providing a viable alternative to fusion for those suffering from painful and debilitating lumbar spinal stenosis and degenerative spondylolisthesis.”
The inspections took place at Premia’s U.S. headquarters in Norwalk, Conn., the company’s production facility in Netanya, Israel, and at two clinical sites—Carolina Neurosurgery & Spine Associates and the Cleveland Clinic’s Neurological Institute Center for Spine Health.
“We are grateful to Drs. Coric, Steinmetz, their staff, and the other 35 clinical sites who diligently performed the IDE study to the highest standards,” responded Jeff Withrow, vice president, Clinical and Reimbursement, Premia Spine.
Premia Spine recently completed a prospective, randomized, multi-center FDA investigational device exemption (IDE) clinical trial comparing the two-year clinical and radiographic outcomes and safety pro patients undergoing either a lumbar TOPS facet arthroplasty or a transforaminal lumbar interbody fusion (TLIF). Initial findings from that study “Prospective, Randomized and Controlled Multicenter Study of Posterior Lumbar Facet Arthroplasty for the Treatment of Spondylolisthesis,” were published in the Journal of Neurosurgery Spine, and concluded that lumbar facet arthroplasty with the TOPS device demonstrates a statistically significant improvement versus lumbar fusion in patient-reported outcome measures, a low surgical complication rate, and the ability to maintain motion at the index level while limiting sagittal translation.
The first and only facet joint replacement system for the lumbar spine, TOPS was developed to maintain motion after decompression for patients with lumbar spinal stenosis and degenerative spondylolisthesis. Spinal stenosis and degenerative spondylolisthesis are painful, debilitating and highly prevalent conditions impacting over 100 million people globally1. An estimated 350,000 people undergo lumbar spinal fusion each year for these conditions2, representing a $2 billion annual addressable global market. TOPS won Breakthrough Device Designation from the FDA in 2021.
About Premia Spine
Premia Spine, a medical technology company, aims to improve the lives of chronic leg and back pain patients. Premia Spine products are designed to provide mobility, stability and durability to patients with lumbar spinal stenosis, degenerative spondylolisthesis and related spinal conditions. The TOPS™ System is CE marked but is not yet approved for sale in the United States.
1 Ravindra, V. M., et al. Degenerative Lumbar Spine Disease: Estimating Global Incidence and Worldwide Volume. Global Spine Journal: 2018, Vol 8, Issue 8.
2 2019 Spinal Surgery Update. Orthopedic Network News: Volume 30, Number 4, October 2019.
Clinical Study
28 Feb 2023
Interim two-year data from clinical IDE trial published in Journal Neurosurgery Spine; lumbar facet arthroplasty moves closer to proving TOPS System viable alternative to fusion
NORWALK, Conn.--(BUSINESS WIRE)--Premia Spine, a medical technology company changing the way debilitating chronic leg and back pain is treated, today announced publication of two-year outcomes from the TOPS facet joint replacement system’s clinical trial in the Journal of Neurosurgery Spine. The study, “Prospective, Randomized and Controlled Multicenter Study of Posterior Lumbar Facet Arthroplasty for the Treatment of Spondylolisthesis,” found lumbar facet arthroplasty with the TOPS device demonstrated a statistically significant improvement versus lumbar fusion in all patient-reported outcome measures, a low surgical complication rate, and the ability to maintain motion at the index level while limiting sagittal translation.
The objective of the prospective, randomized, multi-center U.S. Food and Drug Administration (FDA) investigational device exemption (IDE) clinical trial is to compare the two-year clinical and radiographic outcomes and safety pro patients undergoing either a lumbar TOPS facet arthroplasty or a transforaminal lumbar interbody fusion (TLIF). This publication is the first interim comparative analysis of early clinical outcomes and complications from the TOPS IDE trial. The study will help surgeons more accurately counsel patients on the best treatment for lumbar spinal stenosis and degenerative spondylolisthesis.
“The two-year data from this study indicate the TOPS System compares favorably in all respects to outcomes reported in the FDA trial to a single-level TLIF,” said Dr. Dom Coric, principal investigator in the TOPS IDE study and lead author of the publication. “If at the conclusion of the ongoing clinical trial we see continued favorable outcomes, we will be able to conclude that motion preservation with TOPS facet arthroplasty is a viable alternative to fusion in select patients with spinal stenosis and spondylolisthesis for restoring segmental stability while maintaining motion at the affected segment.”
In the publication, 249 patients were evaluated, with 170 patients in the TOPS investigational arm of the clinical trial and 79 in the TLIF group. TOPS demonstrated a statistically significant advantage over fusion in achieving a meaningful improvement in daily function as measured by ODI (93% versus 81% of patients). The facet replacement group also had a lower reoperation rate than the TLIF group (5.9% versus 8.8%). The TOPS patients maintained complete segmental motion at two years versus their pre-operative measurements.
Lumbar facet arthroplasty with the TOPS device demonstrated a low complication rate, significant improvement in all PROMs, and the ability to maintain motion at the index level while limiting sagittal translation. Additional findings suggest that the TOPS device maintains motion at the index surgical level while preventing further sagittal translation.
“We are encouraged by the data presented in this publication, which show promising results for TOPS when compared to TLIF,” said Ron Sacher, CEO, Premia Spine. “We are demonstrating that the TOPS device dramatically improves patients’ quality of life without sacrificing motion at a previously pathologic intervertebral segment. These data further indicate that we are getting closer to our goal of providing a viable alternative to fusion for those suffering from lumbar spinal stenosis and degenerative spondylolisthesis.”
The first and only facet joint replacement system for the lumbar spine, TOPS was developed to provide mobility, stability and durability after decompression for patients with lumbar spinal stenosis and degenerative spondylolisthesis. Spinal stenosis and degenerative spondylolisthesis are painful, debilitating and highly prevalent conditions impacting over 100 million people globally1. An estimated 350,000 people undergo lumbar spinal fusion each year for these conditions2, representing a $2 billion annual addressable global market. TOPS won Breakthrough Device Designation from the US Food and Drug Administration (FDA) in 2021.
About Premia Spine
Premia Spine, a medical technology company, aims to improve the lives of chronic leg and back pain patients with its TOPS™ System. TOPS is designed to provide lasting mobility, stability and durability to patients with lumbar spinal stenosis, degenerative spondylolisthesis and related spinal conditions.
1 Ravindra, V. M., et al. Degenerative Lumbar Spine Disease: Estimating Global Incidence and Worldwide Volume. Global Spine Journal: 2018, Vol 8, Issue 8.
2 2019 Spinal Surgery Update. Orthopedic Network News: Volume 30, Number 4, October 2019.
Clinical ResultClinical Study
100 Deals associated with Orthopedic ONE
Login to view more data
100 Translational Medicine associated with Orthopedic ONE
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 06 Oct 2024
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or
Translational Medicine
Boost your research with our translational medicine data.
login
or
Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or
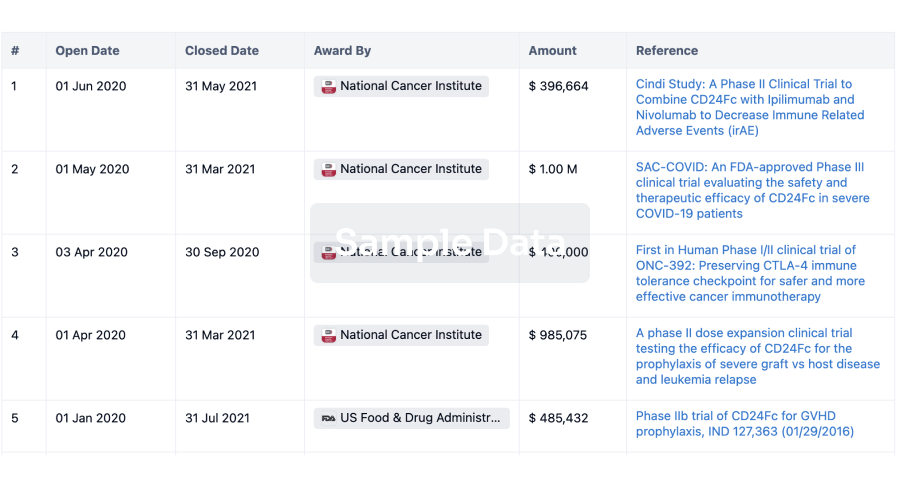
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
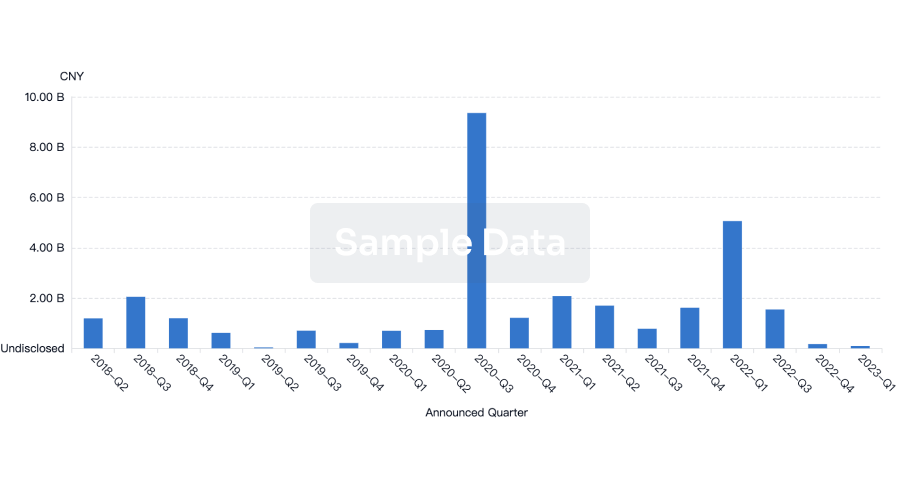
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or
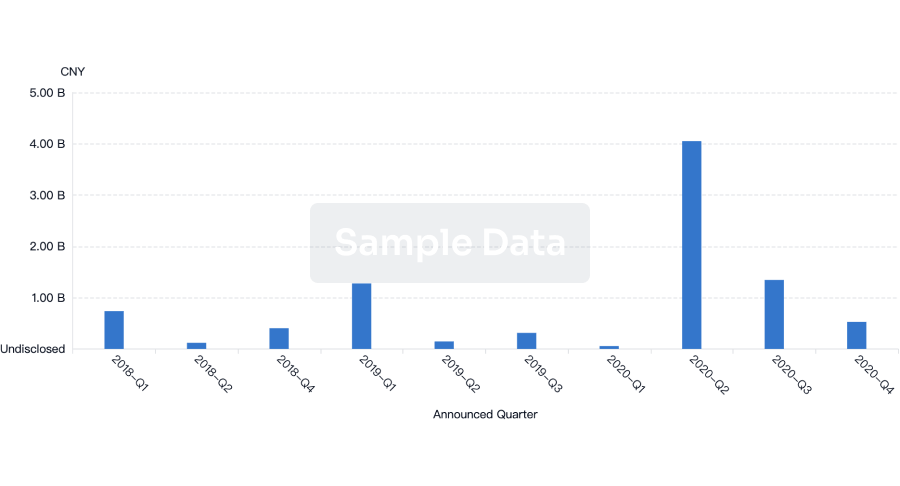
Financing
Unearth financing trends to validate and advance investment opportunities.
login
or
Chat with Hiro
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free