Last update 06 Oct 2024
National Cardiology Hospital
Hospital|
Bulgaria
Hospital|
Bulgaria
Last update 06 Oct 2024
Overview
Related
3
Clinical Trials associated with National Cardiology HospitalEchocardiographic Assessment and CLInical imPlication of Functional tricuSpid rEgurgitation in Heart Failure With Reduced or Preserved Ejection Fraction (ECLIPSE-HF)
Purpose Functional tricuspid regurgitation (FTR) has been shown to be associated with increased morbidity and mortality in several clinical conditions, including heart failure (HF) with reduced left ventricular ejection fraction as well as pulmonary arterial hypertension (PAH). We have designed a study aiming at: characterizing the echocardiographic morphology of the tricuspid valve apparatus and the pathophysiology of FTR in heart failure with reduced, mid-range or preserved left ventricular ejection fraction (HFrEF, HFmrEF, HFpEF) and in PAH patients; correlating the morphologic characteristics of tricuspid valve apparatus with hemodynamic severity of FTR; correlating the severity of FTR with the clinical condition and outcome. Methods The study will be a non-interventional, prospective, international, multicenter, longitudinal study. The minimum number of patients which are expected to be enrolled is 300 HF patients, including HFrEF, HFmrEF and HFpEF patients, whereas 100 PAH patients will serve as control. The patients will be enrolled in 20 centers in Europe, North America and Saudi Arabia. The echocardiographic parameters will be analyzed by the local investigators; a quality control committee will evaluate all data entered in the database to identify potential outliers and a random sample of 10% of cases will be blindly re-analysed in a central core-lab. Conclusions This study has been designed to improve our understanding of pathophysiological mechanisms and clinical relevance of FTR across all HF phenotypes. The results could potentially allow a more appropriate selection of heart failure patients with FTR for tricuspid valve intervention by percutaneous or surgical repair or replacement.
Start Date11 Nov 2021 |
Sponsor / Collaborator |
Strategy To Optimize PeriproCeduraL AnticOagulation in Structural Transseptal Interventions (STOP CLOT Trial) - STOP CLOT
Start Date24 Sep 2021 |
Sponsor / Collaborator |
Morbidity research of traditional Chinese medicine patterns as related to conventional medicine diseases: An observational study on systemic arterial hypertension
Start Date06 Jan 2009 |
Sponsor / Collaborator |
100 Clinical Results associated with National Cardiology Hospital
Login to view more data
0 Patents (Medical) associated with National Cardiology Hospital
Login to view more data
40
Literatures (Medical) associated with National Cardiology Hospital25 Apr 2024·The New England journal of medicine
Empagliflozin after Acute Myocardial Infarction
Article
Author: Jones, W Schuyler ; Zwiener, Isabella ; Mattheus, Michaela ; Gotcheva, Nina ; Udell, Jacob A ; Amir, Offer ; Sumin, Mikhail ; Anker, Stefan D ; Butler, Javed ; Schou, Morten ; Steg, P Gabriel ; Bayes-Genis, Antoni ; van der Meer, Peter ; Petrie, Mark C ; Jeong, Myung Ho ; Rossello, Xavier ; Brueckmann, Martina ; Chopra, Vijay K ; Vinereanu, Dragos ; Goodman, Shaun G ; Ge, Junbo ; Bahit, M Cecilia ; Goto, Shinya ; Hernandez, Adrian F ; Januzzi, James L ; Parkhomenko, Alexander ; Chen, Yundai ; Figtree, Gemma ; Jamal, Waheed ; Szachniewicz, Joanna ; Simic, Dragan ; Parikh, Puja B ; Bhatt, Deepak L ; Harrington, Josephine ; Lopatin, Yuri ; Zieroth, Shelley ; Ponikowski, Piotr ; Bauersachs, Johann ; Merkely, Béla ; Gasior, Tomasz ; Lopes, Renato D
BACKGROUND:
Empagliflozin improves cardiovascular outcomes in patients with heart failure, patients with type 2 diabetes who are at high cardiovascular risk, and patients with chronic kidney disease. The safety and efficacy of empagliflozin in patients who have had acute myocardial infarction are unknown.
METHODS:
In this event-driven, double-blind, randomized, placebo-controlled trial, we assigned, in a 1:1 ratio, patients who had been hospitalized for acute myocardial infarction and were at risk for heart failure to receive empagliflozin at a dose of 10 mg daily or placebo in addition to standard care within 14 days after admission. The primary end point was a composite of hospitalization for heart failure or death from any cause as assessed in a time-to-first-event analysis.
RESULTS:
A total of 3260 patients were assigned to receive empagliflozin and 3262 to receive placebo. During a median follow-up of 17.9 months, a first hospitalization for heart failure or death from any cause occurred in 267 patients (8.2%) in the empagliflozin group and in 298 patients (9.1%) in the placebo group, with incidence rates of 5.9 and 6.6 events, respectively, per 100 patient-years (hazard ratio, 0.90; 95% confidence interval [CI], 0.76 to 1.06; P = 0.21). With respect to the individual components of the primary end point, a first hospitalization for heart failure occurred in 118 patients (3.6%) in the empagliflozin group and in 153 patients (4.7%) in the placebo group (hazard ratio, 0.77; 95% CI, 0.60 to 0.98), and death from any cause occurred in 169 (5.2%) and 178 (5.5%), respectively (hazard ratio, 0.96; 95% CI, 0.78 to 1.19). Adverse events were consistent with the known safety profile of empagliflozin and were similar in the two trial groups.
CONCLUSIONS:
Among patients at increased risk for heart failure after acute myocardial infarction, treatment with empagliflozin did not lead to a significantly lower risk of a first hospitalization for heart failure or death from any cause than placebo. (Funded by Boehringer Ingelheim and Eli Lilly; EMPACT-MI ClinicalTrials.gov number, NCT04509674.).
14 Jul 2023·Diagnostics (Basel, Switzerland)
Surgical Anatomy of the Liver-Significance in Ovarian Cancer Surgery.
Review
Author: Selçuk, Ilker ; Dineva, Svetla ; Watrowski, Rafał ; Kornovski, Yavor ; Slavchev, Stanislav ; Dzhenkov, Deyan ; Kostov, Stoyan ; Yordanov, Angel ; Ivanova, Yonka
INTRODUCTION:
Ovarian cancer is the leading cause of death among all gynecological malignancies. Most patients present with an advanced stage of the disease. The routes of spread in ovarian cancer include peritoneal dissemination, direct invasion, and lymphatic or hematogenous spread, with peritoneal and lymphatic spread being the most common among them. The flow direction of the peritoneal fluid makes the right subphrenic space a target site for peritoneal metastases, and the most frequently affected anatomical area in advanced cases is the right upper quadrant. Complete cytoreduction with no macroscopically visible disease is the most important prognostic factor.
METHODS:
We reviewed published clinical anatomy reports associated with surgery of the liver in cases of advanced ovarian cancer.
RESULTS:
The disease could disseminate anatomical areas, where complex surgery is required-Morrison's pouch, the liver surface, or porta hepatis. The aim of the present article is to emphasize and delineate the gross anatomy of the liver and its surgical application for oncogynecologists. Moreover, the association between the gross and microscopic anatomy of the liver is discussed. Additionally, the vascular supply and variations of the liver are clearly described.
CONCLUSIONS:
Oncogynecologists performing liver mobilization, diaphragmatic stripping, and porta hepatis dissection must have a thorough knowledge of liver anatomy, including morphology, variations, functional status, potential diagnostic imaging mistakes, and anatomical limits of dissection.
01 Jul 2023·Radiology case reports
Disorder of sexual development, urinary bladder duplication, pancake kidney and neural tube defect.
Author: Landzhov, Boycho ; Gaydarski, Lyubomir ; Dineva, Svetla
Congenital malformations of the urogenital system with fully developed duplications, such as urinary bladder, are sporadic. They are often present in the setting of endogenous molecular disbalance, such as steroid metabolism disturbances. Other rare manifestations of hormonal disbalance present as intersex conditions in which the individual has karyotype-specific internal genital organs with opposite-sex signs of the external genitalia, known as ambiguous genitalia. Congenital variations and malformations are often fully recognized and understood during radiological exams. Herein we present a unique case of a 2-month-old baby with female chromosomal sex and ambiguous genitalia together with the manifestation of several anatomical malformations: urinary bladder duplication in the coronal plane, pancake kidney with supernumerary renal arteries, 2 ureters and neural tube defect. Despite their low incidence rate, knowledge of such malformations is paramount for correct diagnosis and treatment in such cases.
2
News (Medical) associated with National Cardiology Hospital18 Nov 2022
DUBLIN, Ireland--(
BUSINESS WIRE
)--CroíValve has announced the successful First in Human implants of its DUO Tricuspid Coaptation Valve technology for the treatment of Tricuspid Regurgitation as part of its TANDEM I study in Poland. The procedures were performed as part of an ongoing clinical trial at the National Institute of Cardiology, Warsaw by Prof Adam Witkowski and Dr Maciej Dąbrowski and the Medical University of Silesia in Katowice by Prof Wojciech Wojakowski.
Tricuspid Regurgitation (TR) is a severe heart condition that occurs when the tricuspid valve, on the right side of the heart, fails to close properly. This results in blood being pumped backwards into the right atrium and venous system causing debilitating symptoms. The DUO System consists of a coaptation valve implant that works in tandem with the native tricuspid valve to restore valve function. The device is delivered using minimally invasive techniques and is secured using a novel anchor system which leaves the frail right heart chamber and native valve apparatus untouched. The implant procedure is straightforward, uses standard imaging and is suitable for a broad patient cohort, including those who are challenging to treat with other valve repair and replacement technologies.
These early cases demonstrate that the DUO System is highly effective at treating TR and significantly improves patients’ symptoms. This is achieved with a straightforward, short procedure, that is easy for the patient to tolerate and for the physician to perform.
“
The DUO System is unique in providing a solution that can effectively treat the dilated right heart anatomy that accompanies Tricuspid Regurgitation, while avoiding contact with the right heart to maintain normal cardiac motion
,” commented Prof Adam Witkowski. “
After 30 days, our patient has already experienced a transformative improvement in symptoms, highlighted by the KCCQ Quality of Life survey and a reduction from NYHA III to NYHA II and significant improvement in 6MWT. In addition, the device continues to exhibit excellent efficacy
.”
“
This early use of the DUO System shows it’s an easy to use, safe and effective device
” added Prof Wojciech Wojakowski. “
Even though it was our first use of the DUO System, the procedure was very straightforward, which is highlighted by the short procedure time. It is a stepwise, controlled approach using standard echo and fluoro imaging and allows us treat patients we would otherwise have no option for”
.
"This achievement is an important milestone on our journey to implement the DUO System as the gold standard approach for treating Tricuspid Regurgitation. We'd like to thank the Heart Teams at the National Institute of Cardiology, Warsaw and the Medical University of Silesia in Katowice. We are excited by this early clinical experience in demonstrating a transformative treatment option for these patients."
said Lucy O’Keeffe, CroíValve’s CEO.

AHA
14 Aug 2021
Currently available options for heart-valve replacement are either short-lived or necessitate the patient to endure long-term medication. But Xeltis’s device evolves into a fully functional natural heart valve that can potentially grow with the patient, thereby reducing repeated interventions, the company recently shared with MD+DI. It works through colonization by the patient’s own tissue, through a process called endogenous tissue restoration (ETR).
“[The device] is made of very biocompatible materials and has a specific porous microstructure,” said the company’s CEO, Eliane Schutte. “This enables the patient’s own cells to fill the pores of the device with new and healthy tissue, as part of natural remodeling processes, i.e., the reorganization or renovation of existing tissue,” she explained, adding that as a natural and functional heart valve made of a patient’s own tissue is restored through ETR, the Xeltis heart valve is then resorbed into the body.
Schutte commented that the process can take between six to 12 months to fully colonize the valve and build strong enough tissue that can take over the device functionality.
The device is made of a special class of polymers, based on supramolecular chemistry, Schutte said. “These polymers are then processed into very thin fibers—much thinner than a hair—to form the shape of the heart valve with the porous microstructure that the cells need to make their home,” she said. “The process used is called electrospinning, which consists of using electric charge to draw polymer solutions into threads.”
The Xplore2/Pivotal trial is an FDA-approved Investigational Device Exemption, prospective, non-randomized clinical study to assess safety and efficacy of the restorative pulmonary valve in up to 50 patients, ranging in age from two to 22, who are undergoing right ventricular outflow tract (RVOT) reconstruction.
Schutte said the company is currently enrolling patients. “Since RVOT reconstruction is luckily required in a relatively small number of children, it may take time to fully enroll the number of patients needed for this trial,” she said. “The enrolled patients will be followed for at least one year to secure the data required for submission to FDA.”
Image courtesy of Xeltis Endogenous tissue restoration (ETR).
The trials will be carried out in up to 15 centers in the United States, Europe, and Asia. Some of the locations include Cincinnati Children’s Hospital, Cincinnati, OH; University of Texas Southwestern Medical Center, Dallas, TX; Children’s Hospital Colorado, Aurora, CO; Children’s Hospital Los Angeles CA; University Children’s Hospital, Krakow, Poland; National Cardiology Hospital Sofia Bulgaria; National Heart Institute, Kuala Lumpur, Malaysia.
There are many other applications for the company’s restorative technology platform, Schutte mentioned. Currently, Xeltis focuses on cardiovascular conditions. “Besides heart valves, we are actively working on small-diameter vascular grafts, such as coronary artery bypass grafts and access grafts for patients undergoing dialysis,” she said.
“Considering both applications, our technology has the potential to positively impact the quality of life of millions of people worldwide,” Schutte concluded.
100 Deals associated with National Cardiology Hospital
Login to view more data
100 Translational Medicine associated with National Cardiology Hospital
Login to view more data
Corporation Tree
Boost your research with our corporation tree data.
login
or
Pipeline
Pipeline Snapshot as of 06 Oct 2024
No data posted
Login to keep update
Deal
Boost your decision using our deal data.
login
or
Translational Medicine
Boost your research with our translational medicine data.
login
or
Profit
Explore the financial positions of over 360K organizations with Synapse.
login
or
Grant & Funding(NIH)
Access more than 2 million grant and funding information to elevate your research journey.
login
or
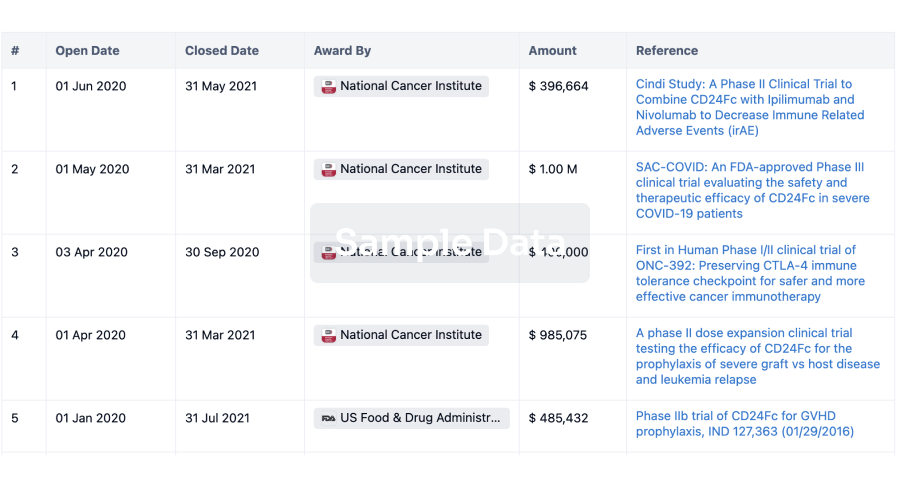
Investment
Gain insights on the latest company investments from start-ups to established corporations.
login
or
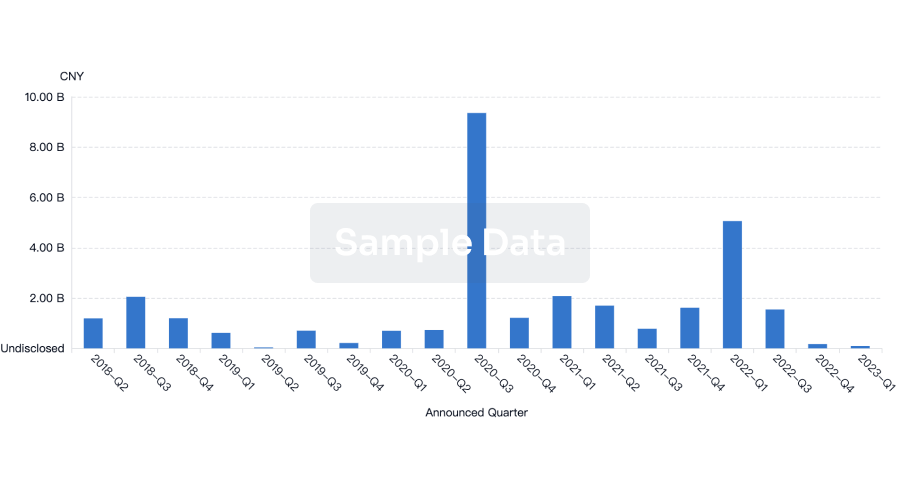
Financing
Unearth financing trends to validate and advance investment opportunities.
login
or
Chat with Hiro
Get started for free today!
Accelerate Strategic R&D decision making with Synapse, PatSnap’s AI-powered Connected Innovation Intelligence Platform Built for Life Sciences Professionals.
Start your data trial now!
Synapse data is also accessible to external entities via APIs or data packages. Empower better decisions with the latest in pharmaceutical intelligence.
Bio
Bio Sequences Search & Analysis
Sign up for free
Chemical
Chemical Structures Search & Analysis
Sign up for free